PULMONARY FUNCTION TEST
EXPERT CARE FOR OPTIMAL LUNG HEALTH AND FUNCTION
Welcome to Atlantic Endocrinology, where we specialize in providing top-tier Pulmonary Function Testing (PFT) services. Understanding your lung health is crucial, and our state-of-the-art testing procedures are designed to do just that. Whether you’re experiencing breathing difficulties, managing chronic lung conditions, or just keen on monitoring your respiratory health, our tests offer detailed insights.
Our team of experienced endocrinologists and respiratory specialists use the latest technology to assess lung function, ensuring accurate diagnosis and effective treatment plans. Embrace a proactive approach to your lung health with Atlantic Endocrinology – where every breath counts.
SCHEDULE YOUR PULMONARY FUNCTION TEST NOW!
YOUR HEALTH, OUR PRIORITY: BENEFITS OF CHOOSING ATLANTIC ENDOCRINOLOGY
- Comprehensive Lung Assessment: Thorough testing for accurate lung health insights.
- Tailored Health Strategies: Personalized treatment plans for various respiratory conditions.
- Advanced Technology: Utilizing the latest in pulmonary testing equipment.
- Experienced Medical Team: Expert care from renowned endocrinologists and respiratory specialists.
- Holistic Approach: Focused not just on treatment but on overall lung health and lifestyle improvements.
OUR PULMONARY FUNCTION TEST DOCTOR
Meet the heart of Atlantic Endocrinology – our dedicated team of endocrinologists, respiratory therapists, and healthcare experts. Each member is committed to providing the highest standard of care, combining years of expertise with a passion for patient health. Our team is your partner in navigating and improving your respiratory health.
WHERE ARE WE LOCATED?
Find Us Easily at New york, Queens – Atlantic Endocrinology, Your Destination for Lung Health Excellence.
Atlantic Endocrinology & Diabetes Center: Dr 1 FL, Rego Park
- 97-25 63 Dr 1 FL, Rego Park, NY 11374
- Monday – Thursday: 9 AM – 7 PM
- Friday: 8 AM – 5 PM
- Saturday: Closed
- Sunday: 8 AM - 6 PM
- +1 (718) 275-2900
Atlantic Endocrinology & Diabetes Center: Rd Suite 103, Queens
- 99-45 67th Rd Suite 103, Forest Hills, NY 11375
- Monday 9 AM – 5 PM
- Tuesday 9 AM – 5 PM
- Wednesday: Closed
- Thursday 9 AM – 5 PM
- Every other Friday 9 AM – 5 PM
- Saturday & Sunday: Closed
- +1 (718) 275-2900
Better Health by Atlantic Endocrinology & Diabetes Clinic
- 97-32 63rd Rd, Rego Park, NY 11374
- Monday – Thursday 9 AM – 7 PM
- Friday: Closed
- Saturday and Sunday: Closed
- (718) 275 - 2900
Here is a short video to talk about pulmonary function test:
WHAT IS A SPIROMETRY?
Spirometry is the most common type of pulmonary function or breathing test. This test measures how much air you can breathe in and out of your lungs, as well as how easily and fast you can blow the air out of your lungs. Your doctor at Atlantic Endocrinology & Diabetes Center may order spirometry if you have wheezing, shortness of breath, or a cough.
It’s carried out using a device called a spirometer, which is a small machine attached by a cable to a mouthpiece.
Spirometry may be performed by a nurse or doctor, or it may be carried out during a short visit to a hospital or clinic.
Spirometry can be used to help diagnose a lung condition if you have symptoms of a problem, or your doctor feels you’re at an increased risk of developing a particular lung condition.
For example, it may be recommended if you have a persistent cough or breathlessness, or if you’re over 35 and smoke.
Conditions that can be picked up and monitored using spirometry include:
• Asthma.
• Chronic obstructive pulmonary disease (COPD).
• Cystic fibrosis.
If you’ve already been diagnosed with a chronic lung disorder, spirometry may be used periodically to check how well your medications are working and whether your breathing problems are under control. Spirometry may be ordered before a planned surgery to check if your lung function is adequate for the rigors of an operation. Additionally, spirometry may be used to screen for occupational-related lung disorders.
WHO IS A CANDIDATE FOR A SPIROMETRY TEST?
A Spirometry test is commonly used for patients with:
• Asthma.
• Shortness of breath.
• Emphysema.
• Chronic cough.
• Chronic obstructive pulmonary disease (COPD).
• Bronchitis.
• Smoking, or exposure to secondhand smoke.
Since the measurement process only takes a few minutes, this allows the patient to discuss the results immediately with their physician. Additional testing may be necessary in order to better diagnose chronic lung conditions such as asthma.
WHAT ARE THE RISKS OF SPIROMETRY?
Generally speaking, a Spirometry is a safe and fairly simple test. Due to the exertion involved, a patient may temporarily feel out of breath or dizzy. For those who have certain heart conditions or may have suffered a recent heart attack, a spirometry may not be performed.
WHAT YOU CAN EXPECT
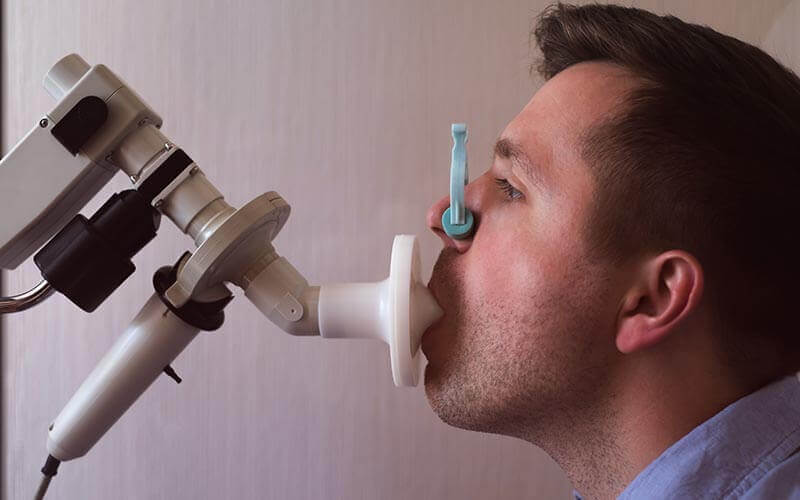
A Spirometry test requires you to breathe into a tube attached to a machine called a spirometer. Before you do the test, a nurse, a technician or your doctor will give you specific instructions. Listen carefully and ask questions if something is not clear. Doing the test correctly is necessary for accurate and meaningful results.
In general, you can expect the following during a spirometry test:
• You’ll likely be seated during the test.
• A clip will be placed on your nose to keep your nostrils closed.
• You will take a deep breath and breathe out as hard as you can for several seconds into the tube. It’s important that your lips create a seal around the tube, so that no air leaks out.
• You’ll need to do the test at least three times to make sure your results are relatively consistent. If there is too much variation among the three outcomes, you may need to repeat the test again. The highest value among three close test results is used as the final result.
Your doctor may give you an inhaled medication to open your lungs (bronchodilator) after the initial round of tests. You’ll need to wait 15 minutes and then do another set of measurements. Your doctor then can compare the results of the two measurements to see whether the bronchodilator improved your airflow.
FREQUENTLY ASKED QUESTIONS (FAQS)
What is a Pulmonary Function Test?
It’s a non-invasive test that measures how well your lungs work.
Why do I need this test?
It helps diagnose lung diseases, measure effects of chronic conditions, and plan treatments.
How should I prepare for the test?
Avoid heavy meals and wearing restrictive clothing; more instructions will be provided upon scheduling.
How long does the test take?
Generally, about 30 to 60 minutes, depending on the tests done.
How often should I have a PFT?
It depends on your health condition; our specialists will recommend a schedule based on your needs.