Osteoporosis, a condition that weakens bones, can be a silent disease. You may not experience any symptoms until a sudden fracture. This is why proactive bone health is crucial.
Consult osteoporosis doctors NYC for trusted expertise!
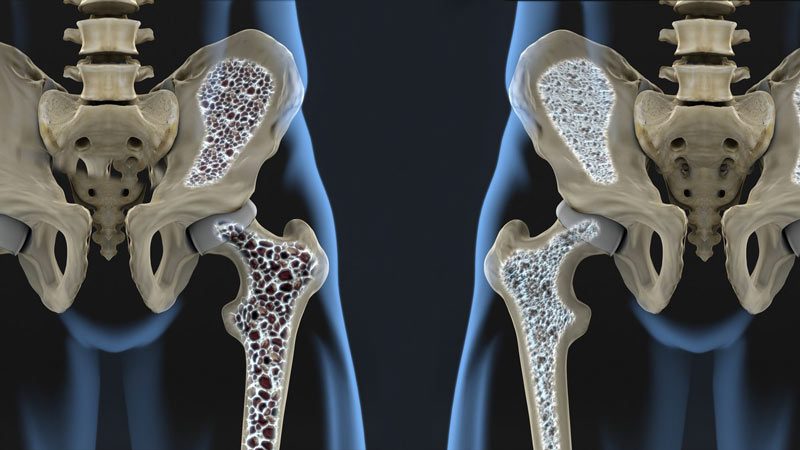
How to Detect Osteoporosis
Since osteoporosis often progresses with no noticeable symptoms, a bone density test is essential. This painless procedure, called DXA (Dual-Energy X-ray Absorptiometry), measures your bone mineral density. The results help doctors diagnose osteoporosis and determine your fracture risk.
Signs That Your Osteoporosis May Be Worsening
1. Increased Fracture Risk
One of the most apparent signs that your osteoporosis may be worsening is an increased risk of fractures. If you experience fractures more frequently, especially in common osteoporotic fracture sites like the hip, spine, and wrist, it’s a clear indication that your bone health is deteriorating.
2. Loss of Height
Osteoporosis can lead to a reduction in height over time due to vertebral compression fractures. If you notice a significant decrease in your height or a stooped posture, it may signal the progression of the condition.
3. Persistent Back Pain
Chronic back pain, especially in the lower back, can be a symptom of vertebral fractures caused by osteoporosis. If you have persistent and unexplained back pain, it’s essential to consult a healthcare professional for evaluation.
4. Decline in Bone Density
Regular bone density scans, often conducted using dual-energy X-ray absorptiometry (DXA), can reveal changes in bone density over time. If your bone density continues to decline in subsequent scans, it suggests worsening osteoporosis.
Monitoring and Managing Osteoporosis
Regular Bone Density Scans
Bone density scans, as mentioned earlier, are essential for monitoring the progression of osteoporosis. These scans can detect changes in bone density and help assess the effectiveness of treatment and lifestyle modifications.
Medications
In some cases, healthcare providers may prescribe medications to manage osteoporosis and reduce the risk of fractures. These medications work by either slowing down bone resorption (breakdown) or promoting bone formation. It’s essential to take these medications as directed and discuss any concerns or side effects with your healthcare provider.
Lifestyle Modifications
Adopting a bone-healthy lifestyle is crucial for managing and slowing down the progression of osteoporosis. This includes:
- Diet: Ensure you have a balanced diet rich in calcium and vitamin D.
- Exercise: Engage in weight-bearing and resistance exercises to strengthen bones and muscles.
- Quit Smoking: If you smoke, quitting is vital for bone health.
- Limit Alcohol: Limit alcohol consumption, as excessive alcohol can weaken bones.
- Prevent Falls: Take measures to prevent falls, such as removing tripping hazards at home and using assistive devices if needed.
Conclusion
Osteoporosis is a progressive condition that requires ongoing attention and management. Recognizing the signs that your osteoporosis may be worsening, such as an increased risk of fractures, loss of height, persistent back pain, or declining bone density, is crucial.
By taking proactive steps, including regular bone density scans, following treatment plans, and adopting a bone-healthy lifestyle, you can effectively manage osteoporosis and reduce the risk of fractures, enhancing your overall bone health and quality of life.