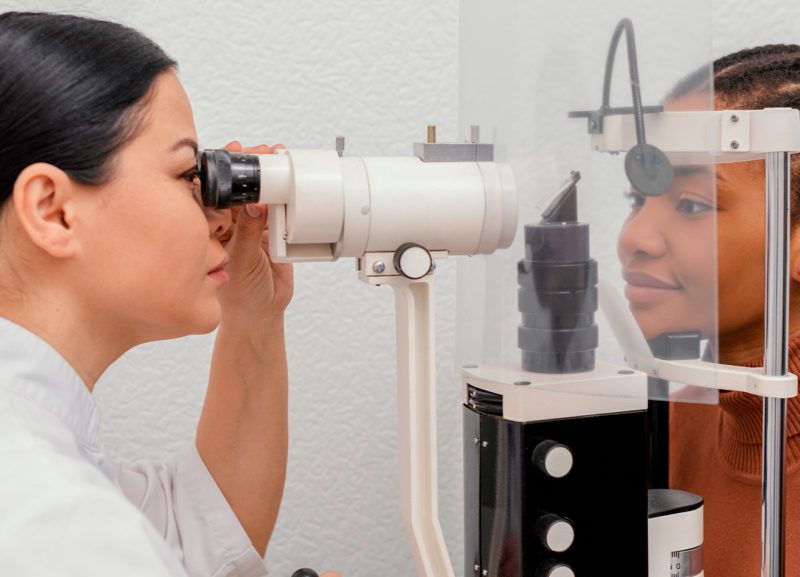
What is Digital Retinal Imaging?
At Atlantic Endocrinology & Diabetes Center a digital retinal imaging, or fundus photography, offers detailed views of the retina, making it easier to detect disease. Early eye disease detection helps ensure that the proper treatment is put in place to hinder disease progression, or cure it all together. Consistently tracking anomalies in the eye with retinal imaging can lead to early detection of the following diseases:
Glaucoma
Retinal imaging can reveal damage to the optic nerve caused by excess pressure or increased pressure on blood vessels in this area. Early detection of glaucoma is crucial, as it can often lead to permanent vision loss for the patient. The Huvitz HFC-1 Non-Mydriatic Fundus Camera includes red-free imaging, which gives a clear comparison of nerve fiber layers to better assist in the diagnosis of glaucoma.
Age-Related Macular Degeneration
Retinal imaging can expose symptoms of age-related macular degeneration, including fluid leakage or bleeding in the rear of the eye. Age-related macular degeneration is one of the primary culprits in vision loss for patients over age 50. Adding retinal imaging to a patient’s eye exam at this age threshold could be the difference between being adequately treated and being oblivious to serious concerns.
Retinal Detachment
For patients who report seeing flashes of light or floaters, you can quickly find evidence that the retina has become detached with retinal imaging. Retinal detachment is a medical emergency that requires prompt treatment to prevent permanent vision loss, so early detection is key.
Diabetic Retinopathy
Patients with diabetes can be screened for early signs of damage to the retina with retinal imaging. Ophthalmologists can also check for other abnormal changes, such as the formation of new blood vessels or leakage in this part of the eye. Swelling in the retina is also a common sign of the disease.
High Blood Pressure
Veins and arteries of the eye are important to observe, especially because they are the only veins and arteries in the body that can be inspected without making an incision. Observation of these veins and arteries can quickly indicate if the patient has high blood pressure. Classic signs of high blood pressure are the blood vessels becoming narrower, bleeding in the rear of the eye, or retinal spots. High blood pressure, or hypertension, can go unnoticed and untreated for months or years, putting the patient at risk for heart problems or stroke.
Cancer
Retinal imaging can significantly increase a patients’ chances of successfully treating certain types of cancer. High-resolution images of the retina can reveal early signs of cancer in the eye, such as dark spots that indicate a melanoma. When these symptoms are noticed early, patients can undergo diagnostic testing and seek treatment promptly to prevent cancer from spreading to other parts of the body. The longer it takes to find and diagnose signs of cancer, the more difficult it becomes to treat, especially if it enters the bloodstream.
Getting in Focus
The most commonly used device for fundoscopy is the standard direct ophthalmoscope, and this procedure can be properly done in a dimly-lit environment. First, the patient’s and doctor’s eyeglasses must be removed, but not contact lenses. It is advisable to give the patient some tissue in case of tearing. The patient is instructed to fix his gaze on the spot around 1 meter ahead. Doctors should refrain from talking with the patient during the procedure, because patients may tend to move their gazes involuntarily. Depending on the eye to be examined, the instrument is then held with the hand belonging to the same side as the examining eye. The patient’s left fundus is examined with the left eye and the right fundus with the right eye. The ophthalmoscope is turned on with the light intensity set at a two-thirds strength and the lens wheel at 0 diopters.
The first step in the fundoscopic procedure is to look for the patient’s red reflex. The patient’s eye is illuminated from a distance of around 12 to 15 inches to examine the red reflex (R/R) of the retina, where the eye appears to glow red. Once this has been achieved, the lens is adjusted to +10 diopters and standing from the patient’s side; the doctor slowly moves toward the patient while looking through the viewing aperture until he is 1-2 inches from the patient’s eye. While moving toward the patient, doctors usually place their hand on the patient’s forehead or shoulder. At +10 diopters, the anterior structures of the eye, such as the cornea, are the first ones to come into focus. Dialing the magnification from +10 to 0 effectively shifts the focus from the front to the back of the patient’s eye, towards the retina.