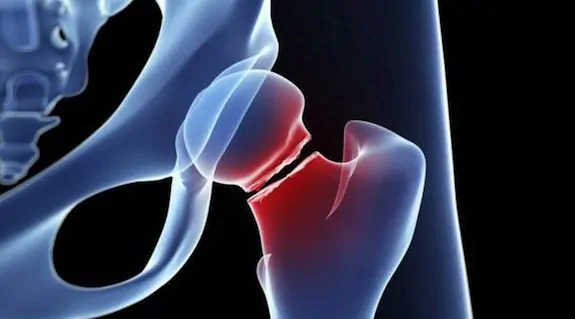
Navigating Bone Fracture Care: Expert Guidance
Experiencing a sudden fall or impact can be alarming, especially if it results in sharp pain and immobility—classic signs of a potential bone fracture. Recognizing who to consult can significantly

Experiencing a sudden fall or impact can be alarming, especially if it results in sharp pain and immobility—classic signs of a potential bone fracture. Recognizing who to consult can significantly
Your endocrine system, often referred to as your body’s “chemical messengers,” plays a vital role in maintaining overall well-being. From regulating metabolism and growth to influencing mood and energy levels,

Hypoglycemia, characterized by low blood sugar levels, can be a concerning condition that affects both individuals with diabetes and those without the condition. Recognizing the signs and understanding the triggers

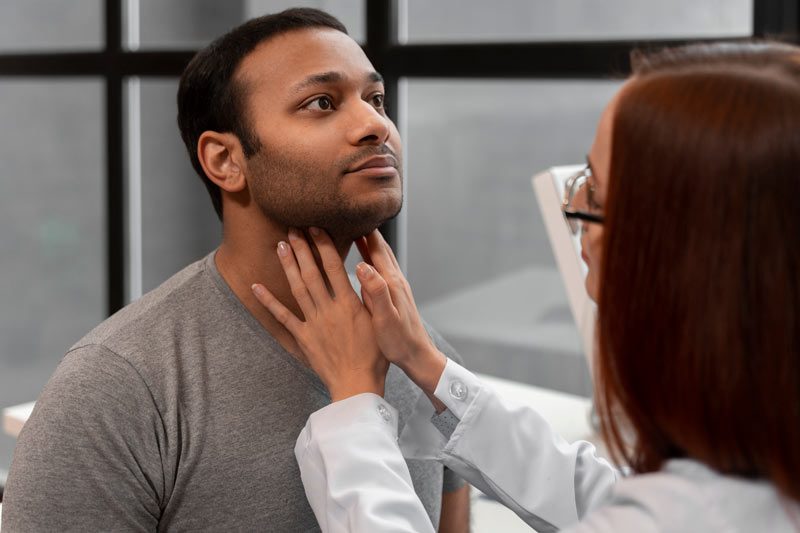
The thyroid gland, a small but mighty organ located in the neck, plays a crucial role in regulating our metabolism, energy levels, and overall well-being. When the thyroid function becomes

At the base of the neck, the thyroid is a butterfly-shaped gland that is crucial in controlling metabolism. Thyroid problems are common and can affect anyone, but women have a
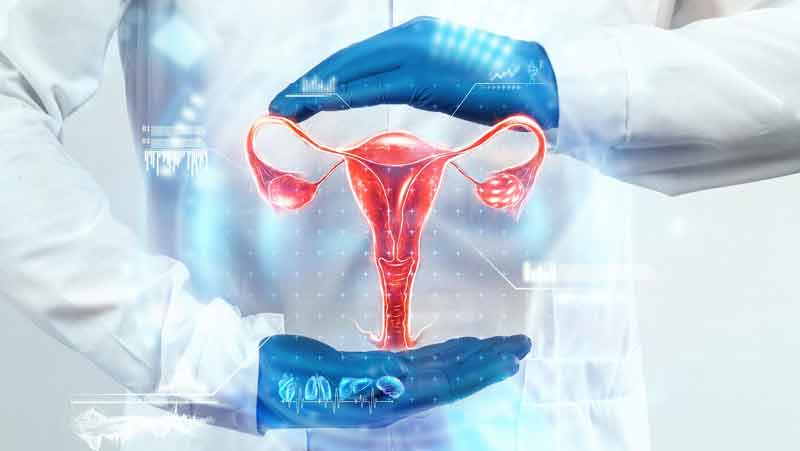
Reproductive endocrinology is a field of medicine that focuses on the hormonal and biological aspects of human reproduction. What Is Reproductive Endocrinology? It involves the study of the complex interactions
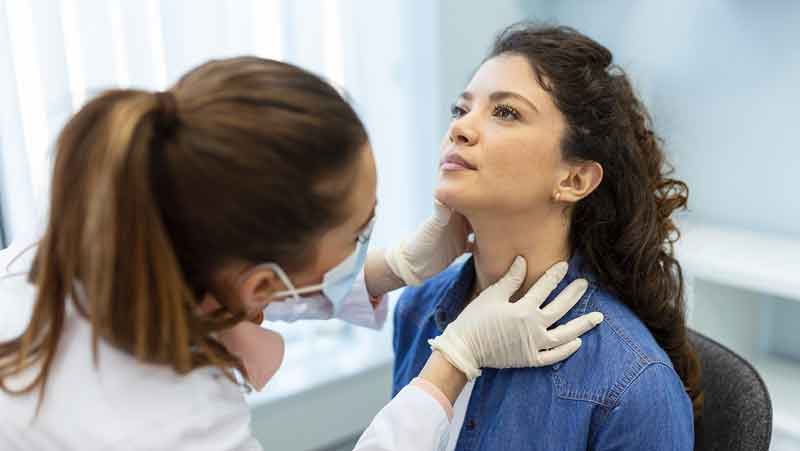
During the first visit to an endocrinologist, the doctor will typically perform a thorough evaluation and assessment to better understand the patient’s symptoms, medical history, and overall health. What does
An endocrinologist is a medical specialist who treats people with a range of conditions that are caused by problems with hormones, such as diabetes, menopause and thyroid problems. Find here
What ismy metabolic type? Your metabolism is how your body converts what you consume into energy for movement and functioning. Think of it in terms of how efficiently your body