Living with hypoglycemia can feel unpredictable—one moment everything seems normal, and the next your body signals that something is off. Many people focus only on blood sugar numbers, but daily habits often play a bigger role than expected. Could small adjustments change how you manage these episodes? With the right Diabetes Management Services in Queens, NY, new strategies for stability may be closer than you think.
TL;DR
Living with hypoglycemia requires recognizing symptoms early and managing blood sugar through consistent daily habits. Key strategies include regular glucose monitoring, balanced meals with complex carbohydrates, protein, and fiber, and safe medication adjustments when needed. Using the 15–15 rule to treat low blood sugar and responding quickly to warning signs can help prevent severe episodes and support more stable glucose control.
Connect with Diabetes Management Services in Queens, NY
What Are Common Symptoms of Hypoglycemia?
Hypoglycemia occurs when blood sugar drops below normal levels, producing physical and emotional symptoms that may appear suddenly. Common signs include trembling, cold sweating, heart palpitations, intense hunger, pale skin, dizziness, and headaches. These symptoms often serve as the body’s first signals that glucose levels need to be restored.
As glucose levels continue to fall, cognitive and emotional symptoms may appear, including confusion, nervousness, anxiety, irritability, or mood changes. Neurological symptoms such as blurred or double vision, difficulty concentrating, slurred speech, weakness, or poor coordination may also occur. These changes can affect the ability to react quickly during an episode.
Severe hypoglycemia may lead to seizures or loss of consciousness. Episodes can also occur during sleep, causing nightmares, nighttime sweating, damp bedding, fatigue, or confusion upon waking. Recognizing these warning signs early allows people to respond before symptoms become more serious.
Monitoring Blood Sugar Levels Regularly
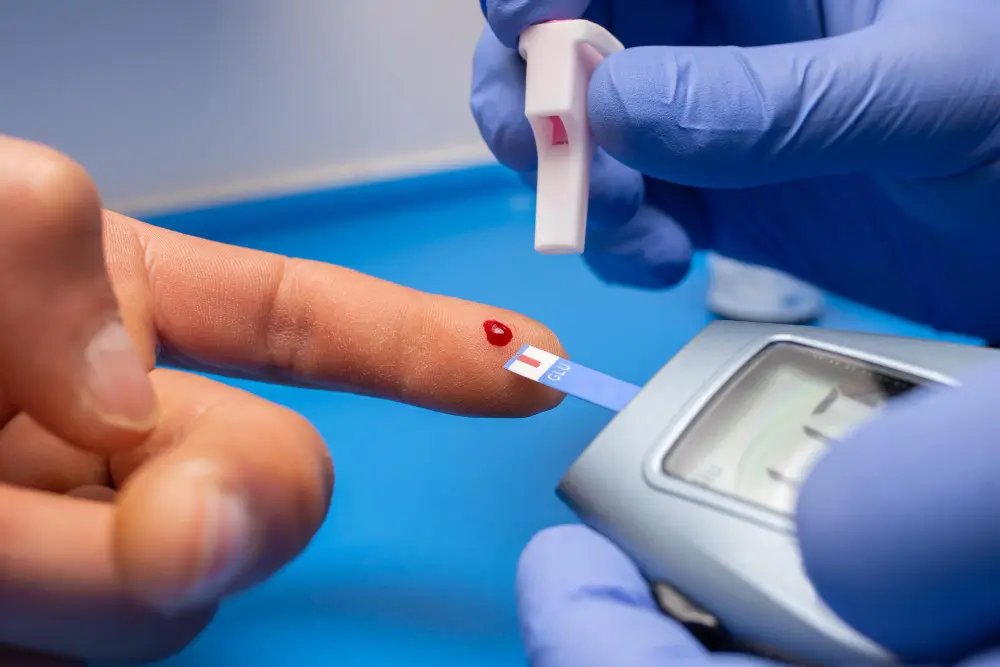
Frequent monitoring of blood sugar levels is a key practice for managing hypoglycemia in daily life. Checking glucose regularly helps detect drops early and allows action before symptoms worsen. Monitoring is particularly recommended before driving, exercising, or when warning signs appear.
Strategies for monitoring and controlling glucose:
- Consistent monitoring: Use a glucometer to check levels regularly, especially when symptoms appear or after intense physical activity.
- Apply the 15–15 rule: If blood sugar is below 70 mg/dL, consume 15–20 grams of fast-acting carbohydrates such as juice or glucose tablets, wait 15 minutes, and measure levels again.
- Meal planning: Maintain regular eating schedules and avoid skipping meals to reduce the risk of glucose drops.
- Preventive snacks: If nighttime hypoglycemia occurs, a small snack before bedtime may help maintain stable levels.
- Technology support: A continuous glucose monitor can alert users to drops in blood sugar, even during sleep.
- Emergency preparation: Carry fast-acting carbohydrates at all times and, if recommended, a glucagon emergency kit for severe situations.
Regular glucose monitoring, combined with consistent eating habits and preparation for possible episodes, can reduce the risk of hypoglycemia. These practices support faster responses to changes in blood sugar and safer daily management.
Planning Balanced Meals and Snacks
Balanced nutrition is a key strategy for managing hypoglycemia in everyday life. Planning meals and snacks carefully helps maintain more stable glucose levels and reduces sudden drops in blood sugar. Combining complex carbohydrates, protein, and fiber supports gradual energy release and may reduce dizziness, fatigue, and other symptoms linked to hypoglycemia.
| Nutritional Element | Role in Glucose Control |
| Complex carbohydrates | Provide slower-releasing energy |
| Protein | Supports satiety and stabilizes glucose |
| Fiber | Promotes slower carbohydrate absorption |
This nutritional balance can help reduce daytime hypoglycemia episodes.
Recommended eating practices:
- Meal frequency: Eat five or six smaller meals daily instead of three large meals.
- Nutrient combination: Pair complex carbohydrates with lean proteins or healthy fats for slower absorption.
- Higher fiber intake: Include fiber-rich foods to help regulate glucose levels.
- Consistent meal timing: Maintain regular eating schedules and avoid skipping meals.
These practices distribute energy more evenly during the day. Eating balanced combinations of complex carbohydrates, protein, and fiber every few hours encourages gradual glucose release and supports more stable blood sugar control.
Adjusting Medication or Insulin Safely
Adjusting medication or insulin safely is part of managing hypoglycemia, particularly when low blood sugar episodes occur frequently. In these cases, consultation with an endocrinology specialist may help evaluate possible changes in treatment. Proper adjustments can reduce sudden glucose drops and support more stable daily levels.
Safe measures for adjusting medication or insulin:
- Use the 15–15 rule: If glucose falls below 70 mg/dL, consume 15–20 grams of fast-acting carbohydrates such as glucose tablets or about 120 ml of non-diet juice or soda. Wait 15 minutes and check levels again. Repeat if necessary.
- Dose adjustments: Recurring hypoglycemia may require reducing insulin doses or modifying medications. One approach involves adjusting morning insulin based on glucose levels before dinner and adjusting nighttime insulin based on morning readings.
- Exercise monitoring: Physical activity may require additional glucose monitoring. Some individuals may need to reduce insulin doses or increase carbohydrate intake before or after exercise.
- Avoid factors that increase insulin absorption: Avoid injecting insulin into muscles that will be heavily used and avoid hot baths immediately after injection.
- Alcohol caution: Avoid alcohol if frequent hypoglycemia episodes occur.
- Emergency preparation: Severe cases involving loss of consciousness may require glucagon administration. If glucose levels remain low after two attempts using the 15–15 rule, medical care should be sought.
Medication and insulin adjustments require careful monitoring and proper medical evaluation. With consistent follow-up, glucose levels can remain more stable.
Recognizing Early Warning Signs
Recognizing early signs of hypoglycemia helps prevent blood sugar from dropping to dangerous levels. When glucose falls below 70 mg/dL, the body may show physical, emotional, and sensory symptoms that signal the change. Identifying these signs quickly allows a fast response, such as consuming sugar using the 15 rule.
Early warning signs include:
- Physical symptoms: Trembling, cold or sticky sweating (often around the neck), rapid heartbeat, dizziness, weakness, intense hunger, pale skin, and headaches.
- Behavioral or cognitive changes: Nervousness, anxiety, irritability, sudden mood changes, confusion, or difficulty concentrating.
- Sensory changes: Blurred or double vision and tingling or numbness in the lips, tongue, or cheeks.
- Sleep-related signs: Nightmares, crying episodes, or excessive sweating during sleep.
If blood sugar continues to drop, severe symptoms such as confusion, vision problems, seizures, or loss of consciousness may occur. Paying attention to these changes supports faster action and safer daily management.
Responding Quickly to Low Blood Sugar
When blood sugar falls below 70 mg/dL, quick action helps prevent symptoms from worsening. The 15–15 rule is a common strategy used to treat hypoglycemia: consume 15–20 grams of fast-acting carbohydrates, wait 15 minutes, then check glucose levels again.
Fast-acting carbohydrate options include three or four glucose tablets, half a cup (120 ml) of fruit juice or regular soda, one tablespoon of sugar or honey, or a tube of glucose gel. These options help raise blood sugar quickly. If levels remain low after 15 minutes, repeat the process.
After glucose returns to a stable range, a small snack may help prevent another drop. Foods high in fat or diet products are not recommended during initial treatment because they do not raise glucose quickly. Severe symptoms or persistent low levels require medical attention.
Key Takeaways
- Recognizing hypoglycemia symptoms early helps prevent severe episodes: Hypoglycemia occurs when blood sugar drops below normal and can cause symptoms such as trembling, sweating, hunger, dizziness, and headaches. As levels continue to fall, cognitive and neurological symptoms like confusion, blurred vision, or difficulty concentrating may appear. Identifying these warning signs early allows people to act quickly and avoid complications such as seizures or loss of consciousness.
- Regular blood sugar monitoring supports safer daily management: Checking glucose levels frequently helps detect drops before symptoms worsen, especially before driving, exercising, or when warning signs appear. Tools like glucometers and continuous glucose monitors can help track levels throughout the day. Being prepared with fast-acting carbohydrates and emergency options can improve response time during low-sugar episodes.
- Balanced meals and consistent eating habits help stabilize glucose levels:
Eating regular meals and snacks that combine complex carbohydrates, protein, and fiber can provide steady energy and reduce sudden drops in blood sugar. Consuming smaller meals several times per day and maintaining consistent meal times may help distribute energy more evenly. These nutritional strategies support more stable glucose control and reduce hypoglycemia risk. - Safe medication or insulin adjustments require careful monitoring: When low blood sugar episodes occur frequently, medication or insulin doses may need to be adjusted with medical guidance. Monitoring glucose levels during exercise, avoiding alcohol in certain situations, and being aware of factors that affect insulin absorption are part of safer management. Emergency options such as glucagon may be necessary in severe cases.
- Responding quickly to low blood sugar can prevent serious complications: The 15–15 rule is commonly used to treat hypoglycemia: consume 15–20 grams of fast-acting carbohydrates, wait 15 minutes, and check glucose again. If levels remain low, the process should be repeated. After recovery, eating a small snack can help maintain stable glucose and prevent another drop.
Sources
- Chatwin, H., Broadley, M., Jensen, M. V., Hendrieckx, C., Carlton, J., Heller, S., … & Pouwer, F. (2021). ‘Never again will I be carefree’: a qualitative study of the impact of hypoglycemia on quality of life among adults with type 1 diabetes. BMJ open diabetes research & care, 9(1).
https://drc.bmj.com/content/9/1/e002322
- Lega, I. C., Yale, J. F., Chadha, A., Paty, B., Roscoe, R., Snider, M., … & Sherifali, D. (2023). Hypoglycemia in adults. Canadian Journal of Diabetes, 47(7), 548-559.
https://www.canadianjournalofdiabetes.com/article/S1499-2671(23)00189-2/fulltext
FAQs
Which fruits are good for diabetes?
People with diabetes can include fruits such as berries, apples, pears, and citrus fruits because they contain fiber and generally have a lower glycemic impact. These fruits help reduce rapid spikes in blood sugar. Fruits with a higher glycemic index, like watermelon, pineapple, ripe bananas, or mangoes, should be eaten in moderation or combined with protein or healthy fats such as nuts or yogurt.
Should I worry if my glucose is 110?
A fasting glucose level of 110 mg/dL is considered elevated and falls within the prediabetes range (100–125 mg/dL). This means the body may not be managing blood sugar as efficiently as it should. While it is not diabetes, it can serve as an early warning sign that lifestyle changes, such as improved diet and regular physical activity, may help reduce the risk of developing type 2 diabetes.
What should a diabetic with high blood pressure eat?
A person with diabetes and high blood pressure can benefit from a balanced diet that includes fruits, vegetables, whole grains, legumes such as beans and peas, and low-fat dairy products. These foods provide fiber and nutrients that support overall health. Choosing balanced meals and limiting less nutritious options may help maintain better control of blood sugar and blood pressure.
What is a prediabetic blood count?
Prediabetes is identified through a blood test that measures HbA1c, which reflects average blood sugar levels over time. An HbA1c result of 41 or lower is considered normal, while 48 or higher may indicate diabetes. Values between 42 and 47 fall into a middle range that suggests an increased risk of developing diabetes in the future.